Our Services
Decision-Grade Intelligence for Health Systems
QALYfAI®
QALYfAI® is HVA’s AI-enabled performance assessment platform. It transforms fragmented clinical, operational, patient-reported and financial data into structured, decision-grade performance profiles.
It converts complexity into accountable evidence.
This enables organisations to:
-
Evidence responsible care delivery
-
Justify funding and network decisions
-
Demonstrate real-world impact
-
Strengthen governance and oversight
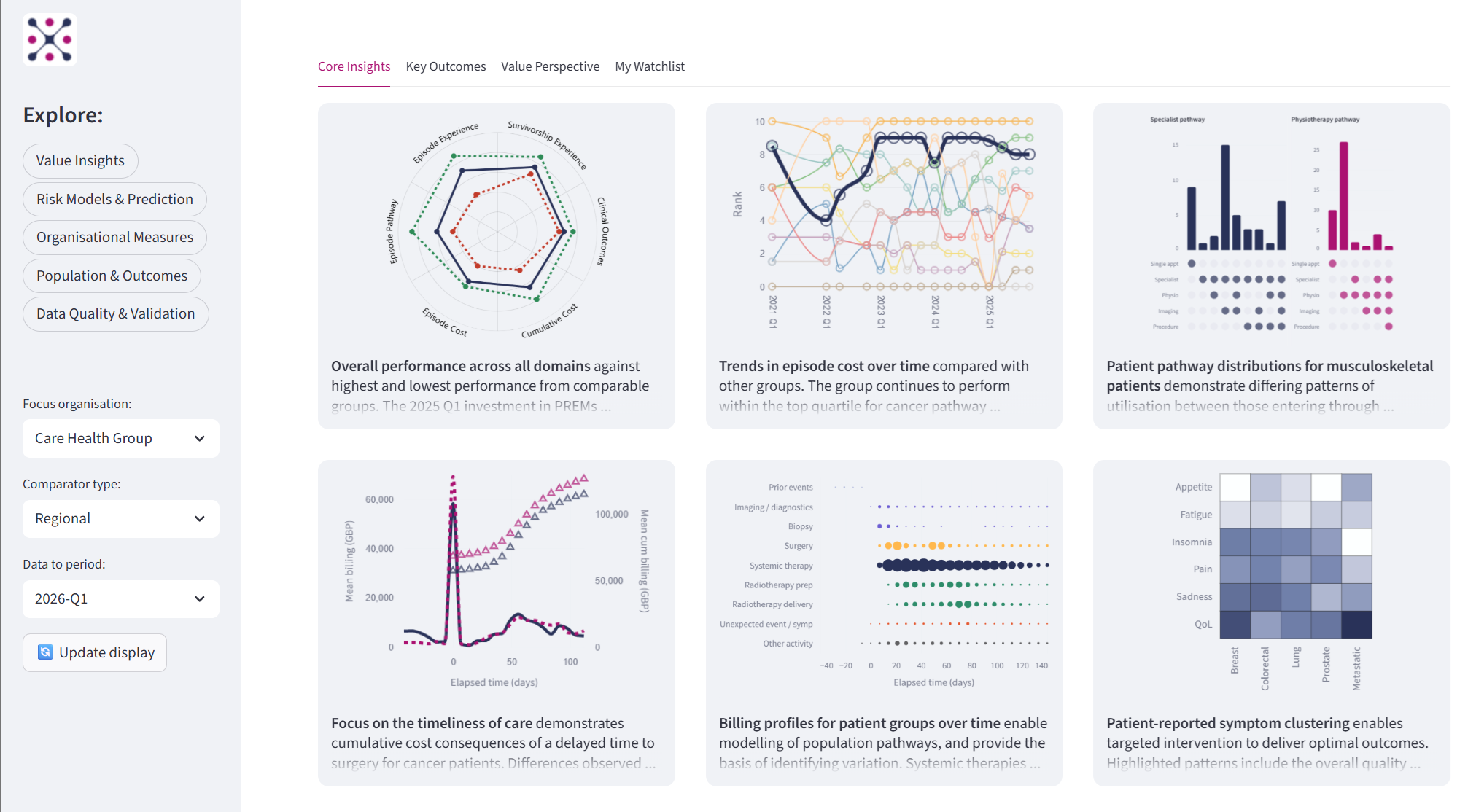
The result is clearer, defensible decision-making — grounded in structured evidence rather than retrospective interpretation.
Who We Support
Payers
Commission sustainable, high-performing care.
Providers
Demonstrate responsible delivery and measurable value.
Innovators
Evidence real-world value in payer-relevant terms.
Regulators & Oversight Bodies
Strengthen governance through integrated performance insight.
Accountable & Value-Based Organisations
Align delivery and funding through system-level evaluation.
Data, Analytics & Actuarial Partners
Strengthen pricing and risk forecasting beyond claims data.
Payers
(Insurers, Health Funds, Employer Plans & Public Purchasers)
Commission sustainable, high-performing care.
QALYfAI® enables payers to commission care based on measurable outcomes, patient experience and long-term financial sustainability — not price signals alone.
It supports payers to:
* Direct patients toward providers delivering sustained value
* Identify financial leakage from fraud, waste, abuse and unwarranted variation
* Strengthen network design through transparent performance benchmarking
* Manage long-term cost exposure, not just episode spend
* Enhance resilience to regulatory and legal scrutiny
Providers
(Hospitals and Clinical Care Providers)
Evidence accountable care and demonstrable value.
QALYfAI® enables providers to link clinical quality and patient outcomes to financial impact — making value visible beyond tariff and activity.
It supports providers to:
* Demonstrate value beyond price and tariff
* Secure network inclusion and sustainable patient volume
* Negotiate performance-linked reimbursement arrangements
* Benchmark against peers and evidence-based standards
* Strengthen clinical governance and payer confidence
Innovators
(Pharma & MedTech)
Demonstrate real-world value in payer-relevant terms.
Trial efficacy alone is insufficient. Payers require evidence that innovations deliver measurable outcomes within sustainable financial parameters. Adoption depends on demonstrable value - not assumption.
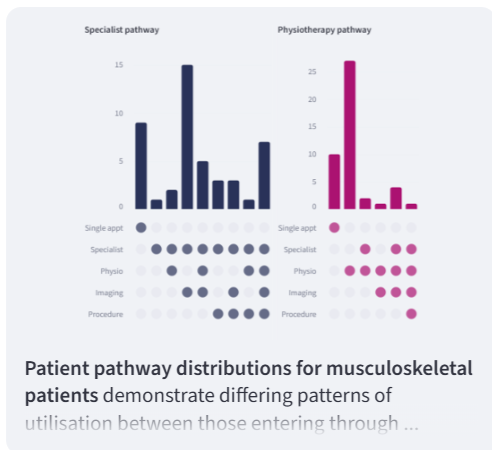
QALYfAI® integrates clinical, patient-reported and claims data to assess how therapies and technologies perform within real-world commissioning environments.
It enables innovators to:
* Demonstrate outcome and cost impact in payer-relevant terms
* Strengthen reimbursement and health technology assessment submissions
* Support value-based pricing and managed access arrangements
* Monitor post-launch performance
Regulators
(Regulatory and Oversight Bodies)
Strengthen oversight through integrated performance insight.
Effective oversight requires commissioning decisions to be grounded in measurable value — not cost control alone. Claims-only analysis cannot assess clinical quality, patient experience or long-term system sustainability.
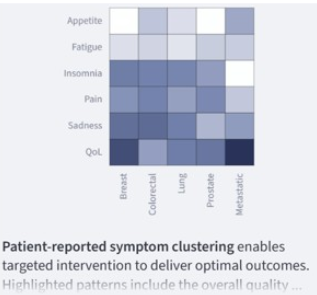
QALYfAI® integrates patient selection, provider and innovation performance, and longitudinal outcome and cost data to generate structured performance insight.
It enables regulators to:
* Evaluate how commissioning decisions perform in practice
* Identify unwarranted variation across hospitals and networks
* Improve transparency across payer–provider systems
* Support proportionate, evidence-based oversight
Accountable, Value-Based & Integrated Care Models
Align delivery and funding through system-level performance evaluation.
Fragmented oversight undermines value-based care. Sustainable integration requires a shared view of clinical performance, patient outcomes and financial impact across care pathways.
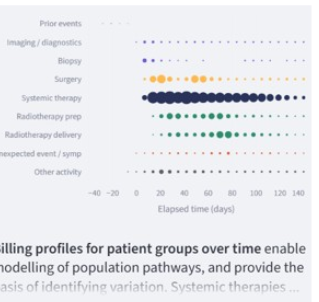
QALYfAI® applies a multidimensional value model linking clinical activity, patient outcomes and experience with longitudinal cost performance across integrated care pathways.
It enables accountable care organisations to:
* Establish a shared performance view across organisations
* Align incentives through outcome and cost transparency
* Support risk-sharing and outcomes-based contracting
* Identify variation across pathways and populations
* Strengthen system-level governance
Data, Analytics & Actuarial Partners
(Actuaries, Health Intelligence & Advanced Analytics Providers)
Strengthen pricing and risk forecasting beyond claims data alone.
Claims data alone cannot capture clinical quality, patient selection, longitudinal outcomes or the full drivers of cost performance.
QALYfAI® enhances actuarial and analytical models by integrating structured performance evidence linking outcomes, cost and funding impact — improving pricing precision, strengthening risk forecasting and increasing confidence in contract performance.
It enables partners to:
* Improve risk forecasting through measurable outcome and cost attribution
* Strengthen pricing accuracy with real-world performance inputs
* Support outcome-linked and risk-share contract design
* Enhance reserving and capital exposure modelling
* Embed broader performance metrics within actuarial frameworks







